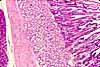
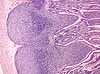
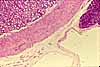
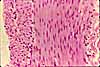
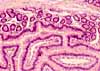
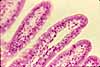
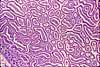
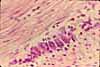
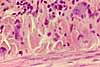
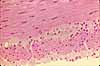
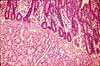
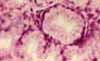
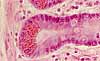
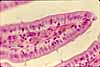
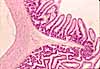
 The mucosa of the small intestine is characterized
by evagination into plicae and villi,
which increase the surface area for nutrient absorption, and by short tubular
invaginations, the crypts, which provide
a protected site for stem cells.
The mucosa of the small intestine is characterized
by evagination into plicae and villi,
which increase the surface area for nutrient absorption, and by short tubular
invaginations, the crypts, which provide
a protected site for stem cells.
The structure of the intestinal mucosa may be altered by pathological processes. Examples include ischemic enteritis or necrotizing enterocolitis, both characterized by necrosis of the mucosa (see WebPath and WebPath), and malabsorption enteropathy (celiac sprue), characterized by blunting or loss of villi with concommitant loss of absorptive surface area, increased crypt length, and inflammatory infiltrate in lamina propria (see WebPath or Milikowski & Berman's Color Atlas of Basic Histopathology, p. 256, or Robbins Pathologic Basis of Disease.)
Cell types of the intestinal mucosa
Small intestinal mucosa is lined by a simple columnar epithelium which consists primarily of absorptive cells (enterocytes), with scattered goblet cells and occasional enteroendocrine cells. In crypts, the epithelium also includes Paneth cells and stem cells.
Functional integrity of the mucosal epithelium is critical for normal function. The cholera toxin kills the epithelial cells, so that cell-to-cell junctions no longer maintain the integrity of the fluid barrier between lumen and lamina propria. As a consequence, bodily fluid moves freely into the lumen and hence out through the intestine as thin watery diarrhea, leading to rapid, massive dehydration and death. Most patients may be saved simply by keeping them hydrated for just a few days, either with an intravenous plasma substitute (expensive) or with a properly balanced solution of salt and sugar delivered orally (cheap). By that time, the cholera vibrios (bacteria) will have cleared, and the epithelium will be replaced by stem cells dividing in the crypts.
Absorptive cells (enterocytes) are responsible for absorbing nutrients from the intestinal lumen and transporting them across the epithelium to the lamina propria, whence they diffuse into capillaries.
The brush border of the intestinal epithelium not only facilitates absorption, it also provides a site of attachment for pathogens. For an example (cryptosporidia), see WebPath.
Goblet cells secrete mucus to promote movement and effective diffusion of gut contents. The proportion of goblet cells generally increases as one progresses down the GI tract, with the highest proportion found in the lower tract.
Enteroendocrine cells (not pictured) secrete hormones to regulate secretion into the GI tract.
Tuft cells (not pictured) orchestrate immunity against parasites.
Paneth cells, located at the bottoms of the crypts, secrete lysosomal enzymes and other factors into the crypt lumen. These agents presumably help protect the crypt epithelium with its vital stem cells.
Stem cells line the walls of the crypts and continually replenish the intestinal epithelium, completely replacing all the absorptive and goblet cells approximately once every four days.
Lamina propria of each villus is richly supplied with capillaries as well as a single lacteal, for transporting absorbed nutrients. Lamina propria also includes thin strands of smooth muscle (presumably allowing some motility for individual villi, to encourage thorough fluid mixing at the absorptive surface) and numerous white blood cells.
The muscularis mucosa of the small intestine forms a thin layer (only a few muscle fibers in thickness) beneath the deep ends of the crypts.
The submucosa of the small intestine is relatively unspecialized, except in the duodenum where it is packed with the mucous-secreting Brunner's glands.
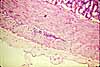 Muscularis externa of the small intestine has the standard layers of inner circular
and outer longitudinal smooth muscle, with
ganglia of Auerbach's plexus scattered
in between.
Muscularis externa of the small intestine has the standard layers of inner circular
and outer longitudinal smooth muscle, with
ganglia of Auerbach's plexus scattered
in between.
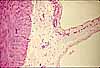 Over most of the small intestine, the outer layer is a serosa
attached to mesentery. The exception
is the duodenum, which is retroperitoneal.
Over most of the small intestine, the outer layer is a serosa
attached to mesentery. The exception
is the duodenum, which is retroperitoneal.