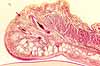
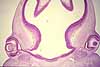
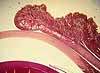
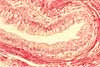
Overview / Basic tissue structure of the eyeball
Beneath a thin conjunctival epithelium, the eyeball consists of three principal layers.
- The outer layer consists of dense fibrous connective tissue.
- This layer includes both sclera and cornea.
- The sclera is the "white" of the eye.
- The sclera is continuous with the transparent substantia propria
of the cornea.
- The next layer, or uvea, includes the choroid,
the ciliary body, and the iris.
- The choroid, lying between sclera and retina, consists of highly vascularized loose connective tissue, heavily pigmented with many melanocytes.
- Smooth muscle of the ciliary body controls the focal length of the lens
- An anterior hole in this layer, the pupil, allows light to pass through.
- The iris controls the size of the pupil.
- A posterior hole in the uvea accommodates the optic nerve.

- The inner layer, or retina, includes two
portions, both formed from an outpouching of the embryonic brain.
- The neural retina is the photoreceptive, imaging-processing tissue.
- The pigmented epithelium lies behind the neural retina; it also extends forward to line the inward side of the iris.

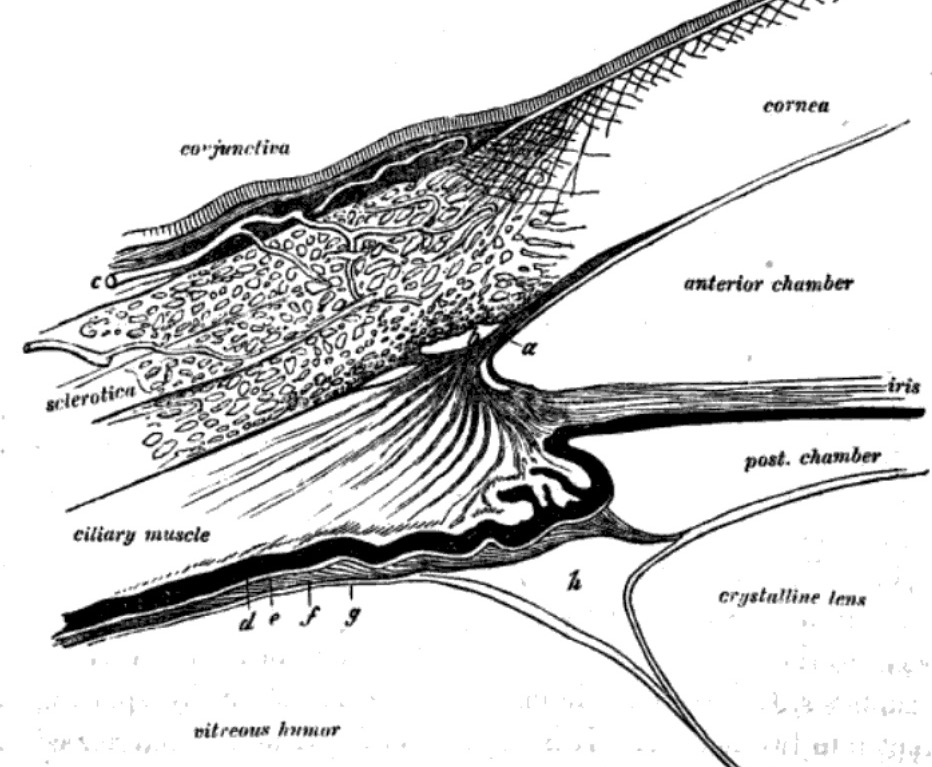
These three layers surround two internal compartments.
- Between the cornea and the iris lies the anterior chamber, filled with a fluid called aqueous humor.
- Behind the iris and lens lies the posterior chamber, filled with clear gelatinous tissue called vitreous humor.
The anterior and posterior chambers are separated by the lens. The lens is a peculiar epithelial structure,
formed from embryonic ectoderm, which is suspended behind the pupil by suspensory fibers.
Sclera

The sclera, or "white" of the eye, is a very simple example of dense, fibrous connective tissue. It reveals, in a visibly obvious way, the intrinsic colorlessness of collagen.
The dense fibrous connective tissue of the sclera is continuous with the dense fibrous connective tissue of the cornea.
At the limbus, where the sclera meets the cornea, extracellular spaces in the connective tissue form the canal of Schlemm. This is the route for aqueous humor to drain from the anterior chamber.

A hole at the back of the sclera accommodates the optic nerve. The sclera is relatively impermeable; blood vessels serving deeper tissues join the optic nerve into the interior of the eye.
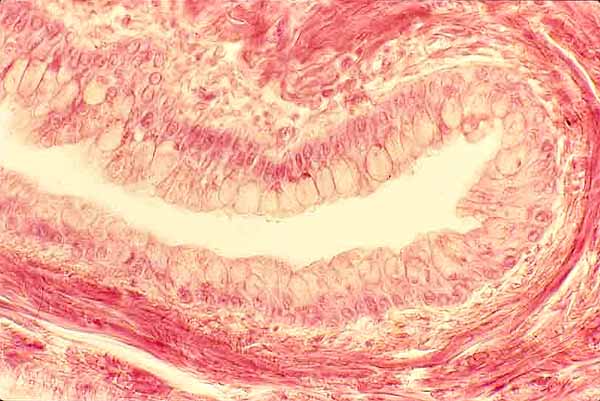
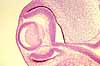
Cornea

The cornea consists of a thin surface of non-keratinized stratified squamous epithelium overlying a layer of dense fibrous connective tissue, called substantia propria.
Although the cornea is composed of the same tissue elements as other body parts (i.e., epithelial cells, collagen, fibroblasts, etc.), the cornea is quite unlike most tissues in that it is perfectly transparent.
Compare and contrast the tissue layers of the cornea with those of other body surfaces:
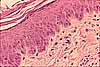 |
 |
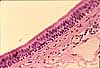 |
The features which distinguish corneal tissues from those of other body surfaces are all related to its transparency.
 The
epithelium of the cornea is continuous with the epithelium of the conjunctiva, which
in turn is continuous with the epidermis of skin on the exposed surface of
the eyelid.
The
epithelium of the cornea is continuous with the epithelium of the conjunctiva, which
in turn is continuous with the epidermis of skin on the exposed surface of
the eyelid.
Corneal epithelium is very thin (only a few cells thick).
Corneal epithelium lies flat against the underlying substantia propria, in contrast with most other examples of stratified squamous epithelium. For example, the base of the epidermis is indented by many connective tissue papillae. (This arrangement in skin presumably helps reinforce epidermal attachment against mechanical stress. Such reinforcement is hardly necessary for the cornea.)
The exceptionally thick basement membrane between corneal epithelium and substantia propria is called Bowman's membrane (named after William Bowman, b. 1816; this is the same Bowman who gives his name to Bowman's capsule of the renal glomerulus).
The substantia propria of the cornea, like most dense fibrous connective tissue, is mostly collagen and ground substance, with fibroblasts as the predominant cell type. (Corneal fibroblasts are also called keratocytes, not to be confused with keratinocytes of epidermis.) Quite unlike most other dense, fibrous connective tissue, the corneal connective tissue is perfectly transparent.
Collagen of the cornea is organized into extremely regular layers. All the collagen fibers in one layer are arranged in parallel, with alternating layers running in different directions.
Corneal connective tissue has no blood vessels. (You don't need a microscope to confirm this; just look in a mirror.)
Even though cells of the cornea are not very active metabolically, they still need oxygen and nutrients. As long as the cornea is in direct contact with air, oxygen can be absorbed directly. Nutrients can diffuse into cornea from aqueous humor.
Cells of corneal connective tissue are mostly fibroblasts (keratocytes). There is no immune-system component, hence the relative ease with which corneal tissue can be transplanted without need for careful tissue typing.
At the inner surface of the cornea is a cellular layer, resembling a simple low cuboidal epithelium, called corneal endothelium. (This is a unique use of the term endothelium; it is not related to vascular endothelium.) Between corneal endothelium and substantia propria is a thick basal lamina called Descemet's membrane (named after Jean Descemet, b. 1732). It is believed that the corneal endothelium is essential for maintaining corneal transparency, by regulating the composition of ground substance in the substantial propria. For recent research, see here (Experimental Eye Research 2020 Aug;197:108090. doi: 10.1016/j.exer.2020.108090).
Clinical note: The surgical procedure of endothelial keratoplasty, to address Fuch's dystrophy, replaces both corneal endothelium and Descemet's membrane with transplant tissue.
Corneal epithelium contains free nerve endings. Since pain seems to be the only sensory modality that functions for corneal tissue, biologists long ago decided that free nerve endings elsewhere might also represent pain fibers.
Corneal transparency.
The tissue elements of the cornea are specialized for transparency. The effectiveness of this design can be readily seen by looking in the mirror and comparing cornea with sclera (the white of the eye). However, apart from the cornea's obvious absence of blood vessels, its tissue composition appears remarkably similar to that of the sclera. Yet unlike the sclera, the cornea is marvellously transparent.
Below is a simplified introduction to the mechanisms underlying corneal transparency. For a fairly recent, detailed review, see Progress in Retinal and Eye Research, Vol. 49, pp. 1-16 (November 2015).
The transparency of the cornea is based primarily on the regularity of its tissue components, which minimizes the number of surfaces where light can be refracted or reflected.

At the limbus (the edge of the cornea, where the cornea meets the sclera), it is apparent that the epithelium of the cornea is quite similar to that of the scleral conjunctiva, except for a less irregular basal boundary with the underlying connective tissue. Similarly, collagen of the corneal substantia propria is not noticably different from collagen of the sclera, except for being slightly more uniform in arrangement. But these small differences are significant; the sclera is opaque while the cornea is transparent.
The effect is rather like the difference between packed snow and crystalline ice -- both have the same composition (frozen water), but one is opaque (by scattering the light off the surfaces of many tiny snow crystals) while the other is crystal clear.
Although most cells and fibers are colorless, their surfaces can scatter light when irregularly arranged. Similarly, light scattered from colorless and transparent ice crystals produce the familiar whiteness of winter snow. Such scattering (together with absorption of light by pigments such as melanin and hemoglobin) prevents light from passing freely through most tissues.
Features of the cornea which minimize the scattering of light include the following:

- Both outer and inner surfaces of the corneal epithelium are smooth.
- The collagen fibers of the substantia propria are arranged into uniform layers with parallel fibers within each layer (unlike the more irregular texture of collagen in the sclera and in the dermis of the skin).
- The water content of the ground substance is carefully regulated, to maintain uniform spacing among collagen fibers.
Collagen fibers are formed extracellularly, self-assembling from tropocollagen molecules (secreted as procollagen by fibroblasts). The regulatory machinery responsible for the regular arrangement of collagen fibers in the cornea remains unknown.
The low cuboidal cells which form the cornea's innermost layer, the so-called corneal endothelium, actively pump ions and water from the corneal ground substance into the aqueous humor, to prevent excess water from disturbing the regularity of the collagen layers and causing opacity.
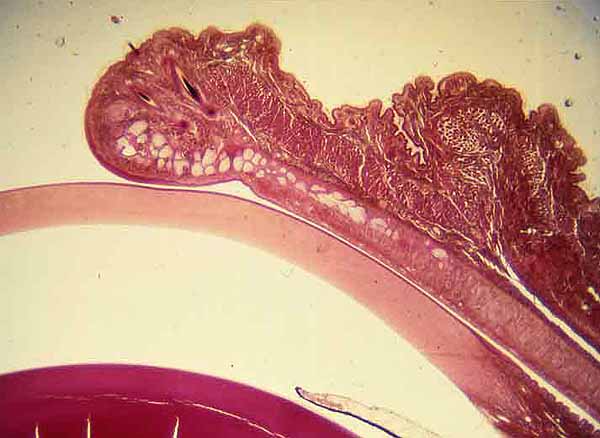
Uvea
The next layer inward from the sclera and cornea is the uvea, which has three portions: iris, ciliary body, and choroid.
- The iris is the variously pigmented loose connective tissue surrounding the pupil.
- The ciliary body is a ring of smooth muscle, located at the base of the iris beneath the limbus.
- The choroid extends around the remainder of the eyeball, except for a hole where the optic nerve passes through to the retina.
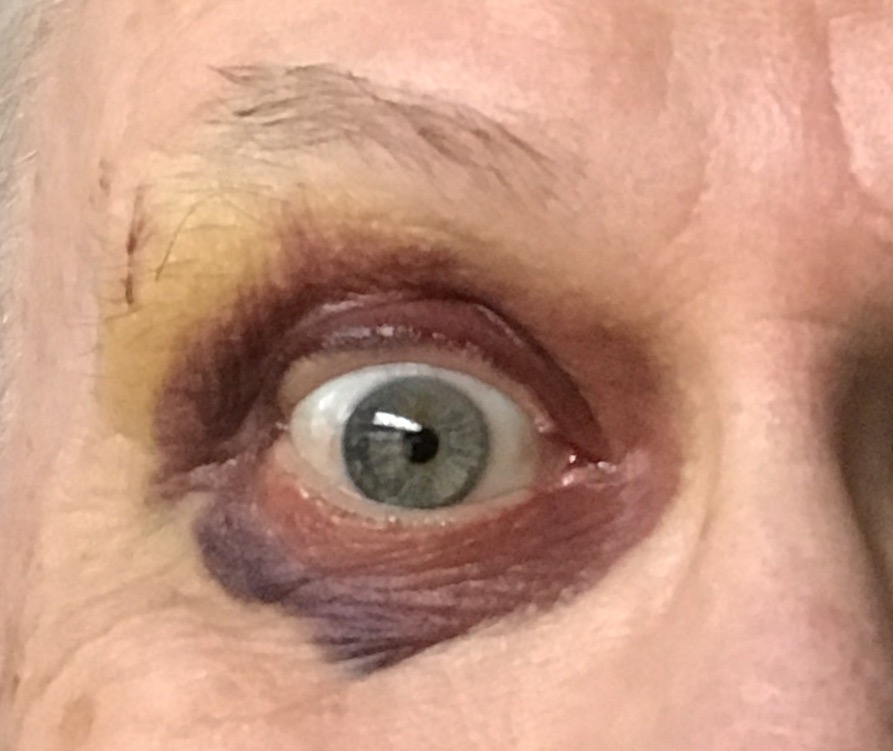
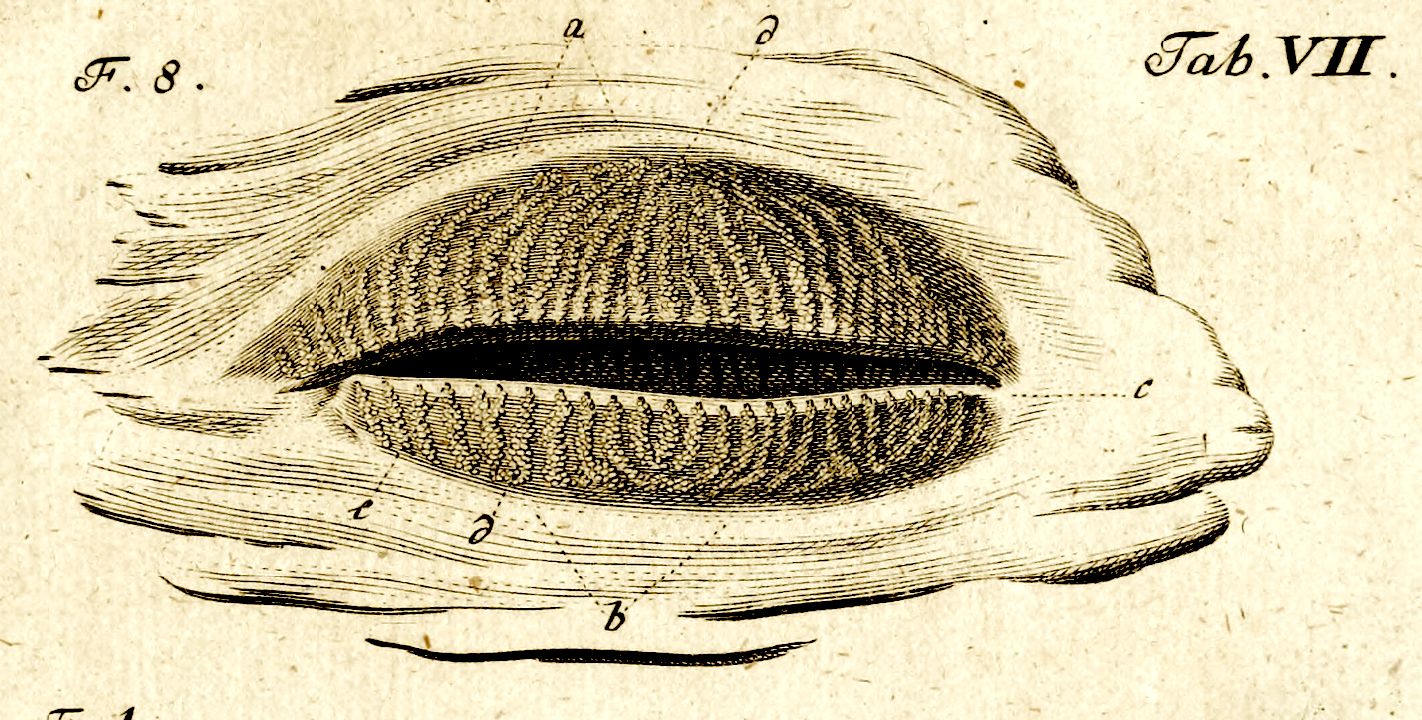
Functionally, the iris is a rather simple opaque ring surrounding and controlling the diameter of its central aperture, the pupil.
However, the iris does have some peculiar histological features.
- The iris is the only internal organ which is clearly visible from outside
the body. The visible surface of the iris consists of loose connective
tissue.
- The color of the iris ("eye color") results both from scattering of light by loosely arranged collagen fibers and from absorption of light by melanin granules in scattered melanocytes.
- Variation in eye color result from individual differences in the distribution
and density of melanocytes and collagen fibers.
- The posterior (hidden) surface of the iris is an intensely pigmented extension
of the embryological optic cup (the same structure which forms the retina
and the pigmented epithelium).
This tissue continues as the ciliary processes
around the perimeter of the iris.

- A ring of smooth muscle surrounding the pupil comprises the pupillary
sphincter.
- The pupillary dilator is not ordinary smooth muscle but rather contractile extensions of myoepithelial cells of the deep layer of the two-layered pigmented epithelial tissue that comprises the posterior surface of the iris.
Choroid

The choroid is a highly vascular, loose connective tissue layer. This layer is packed with melanocytes and thus heavily pigmented, to absorb any stray light that might leak into the eye through the sclera.
Bruch's membrane (commemorating Carl Wilhelm Ludwig Bruch, b. 1819) separates the choroid from the retina. Bruch's membrane is a thin layer of extracellular material that allows diffusion from choroid to nourish the outer layers of the retina. Deterioration of this membrane is associated with age-related macular degeneration. For a review, see Adv. Exp. Med. Biol. (2021) 1256:89-119; doi: 10.1007/978-3-030-66014-7_4.)
Ciliary body
 Deep to the limbus (i.e., the site where the cornea meets
the sclera), the uvea
is thickened into the ciliary body.
Deep to the limbus (i.e., the site where the cornea meets
the sclera), the uvea
is thickened into the ciliary body.
- The ciliary body is a ring of smooth muscle fibers arranged concentrically
around the opening in which the lens is suspended.
- The lens is suspended from the ciliary body by thin suspensory fibers of fibrillin.
 The ciliary body, acting through the suspensory fibers, controls the shape of
the lens.
The ciliary body, acting through the suspensory fibers, controls the shape of
the lens.
- When smooth muscle of the ciliary body is in a relaxed state,
the elasticity ("springiness") of the eyeball puts tension on the suspensory fibers. This stretches the
lens radially, thereby making it thinner. In this condition, the lens brings
distant objects into focus on the retina.
- When smooth muscle of the ciliary body contracts, the diameter of the opening in which
the lens is suspended becomes (slightly) smaller and tension on the suspensory
fibers is relaxed. The lens is then allowed to relax toward its "resting"
shape, which is more round. In this condition, the lens brings nearby
objects into focus on the retina.
- Note that a stretched lens, for distant focus, is maintained by
a relaxed muscle. Hence eyes at rest are focussed for distance
vision.
- Conversely, a contracted muscle is responsible for a relaxed lens, for near focus. Close work is tiring because the ciliary body must remain in contraction to maintain focus.

 Ciliary processes, aqueous humor, and canal of Schlemm
Ciliary processes, aqueous humor, and canal of Schlemm
The surface of the ciliary body is covered by an extension of the embryonic optic cup (the same tissue which forms the neural retina and the pigmented epithelium). Small projections of this tissue form the ciliary processes. The epithelium of the ciliary processes secretes the aqueous humor.
Aqueous humor flows from its site of formation in the posterior chamber (i.e., behind the iris) through the pupil into the anterior chamber. From there it drains into the canal of Schlemm and hence into venous drainage.
This is one of three sites associated with the nervous system where a special fluid is produced by a unique tissue, with this fluid needing an outlet elsewhere to avoid buildup of pressure. (The other two sites are the inner ear and the brain. In the ear, endolymph secreted the by stria vascularis is drained through the endolymphatic sac. In the brain, cerebrospinal fluid secreted by choroid plexus is drained through arachnoid villi into the superior sagittal sinus.) In each of these sites, an imbalance between production and drainage can cause neurological symptoms.
Clinical note: Increased fluid pressure inside the eyeball caused by an imbalance between the formation and drainage of aqueous humor can reduce blood flow into the eyeball, leading to glaucoma.
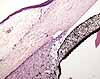
The canal of Schlemm, also called the scleral venous sinus, is a channel associated with a network of connective tissue spaces, the trabecular meshwork, located at the limbus where cornea, sclera, and ciliary body meet. This provides a route through which aqueous humor can escape from the anterior chamber and seep into venous drainage.
A nice diagram may be found here [Acta Ophthalmol. (2022) 100(4): e881-e890; doi: 10.1111/aos.15027].
The traditional name "canal of Schlemm" commemorates Friedrich Schlemm, b. 1795.
Lens and suspensory fibers (zonules)
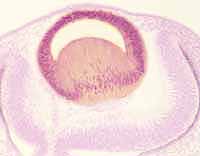
Histologically, the lens is bizarre. It is an isolated island of epithelial tissue with an anterior layer that is simple cuboidal and a posterior layer consisting of extravagantly elongated cells, called lens fibers, that are packed with lens protein. This pattern is most readily understood by considering the embryology of the eye.
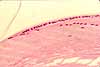
At the edge of the lens, one can see where these two different epithelial cell shapes meet one another.
Mature lens fibers consist almost entirely of protein. Deterioration over time can lead to cataracts. (Historical note: For a poignant description of cataract removal surgery in the era before anesthesia, see the Jacob entry on the histology eponyms page.)
The lens is suspended from the ciliary body by thin suspensory fibers made of fibrillin. These fibers are commonly called zonules, although that terminology is etymologically dubious. More properly the entire web of suspensory fibers forms a band encircling the lens; this is the zonule of Zinn (commemorating Johann Zinn, b. 1727).
 The shape of the lens (and hence its focal length) is determined by tension exerted
through the suspensory fibers, controlled by smooth
muscle of the ciliary body.
The shape of the lens (and hence its focal length) is determined by tension exerted
through the suspensory fibers, controlled by smooth
muscle of the ciliary body.
Retina
The retina consists of two fundamentally distinct layers, the neural retina (often called simply "the retina") and the pigmented epithelium. These two layers derive, respectively, from the front and back ectodermal surfaces of the embryonic optic cup.
 The neural retina is the light-sensitive tissue of the eye.
The neural retina is the light-sensitive tissue of the eye.
The retina is famously built "upside down." That is, the photoreceptor cells (rods and cones) are located in the back of the retina, so light must pass through all of the layers of the neural retina before getting to the receptors.
Even worse, the blood vessels which serve the retina are spread across the front surface, so light on its way to the receptors must also pass by the blood vessels. Our visual system is designed to ignore the blood vessels (as well as anything else whose position on the retina does not move); otherwise every view of the world would have a superimposed array of branching blood vessels and coursing red blood cells.
As one final insult, the nerve fibers which eventually travel from the eye through the optic nerve must pass through the layers of the retina, leaving a "blind spot" where they do so. And once again, our visual system is designed to ignore the blind spot, filling in the corresponding "hole" in the visual field with whatever color and texture does the best job of hiding the blind spot. [ How to "see" your own blind spot. ]
The fovea is a central patch of retina with high acuity. Here the issues noted above are minimized by thinning the layers inward from the photoreceptors, displacing cell bodies, nerve fibers, and blood vessels away from this spot. To accomplish this, axons from photoreceptors are "stretched" to reach connections with bipolar cells in the outer plexiform layer, creating the Henle fiber layer [commemorating Friedrich Henle, 1809-1885].
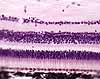
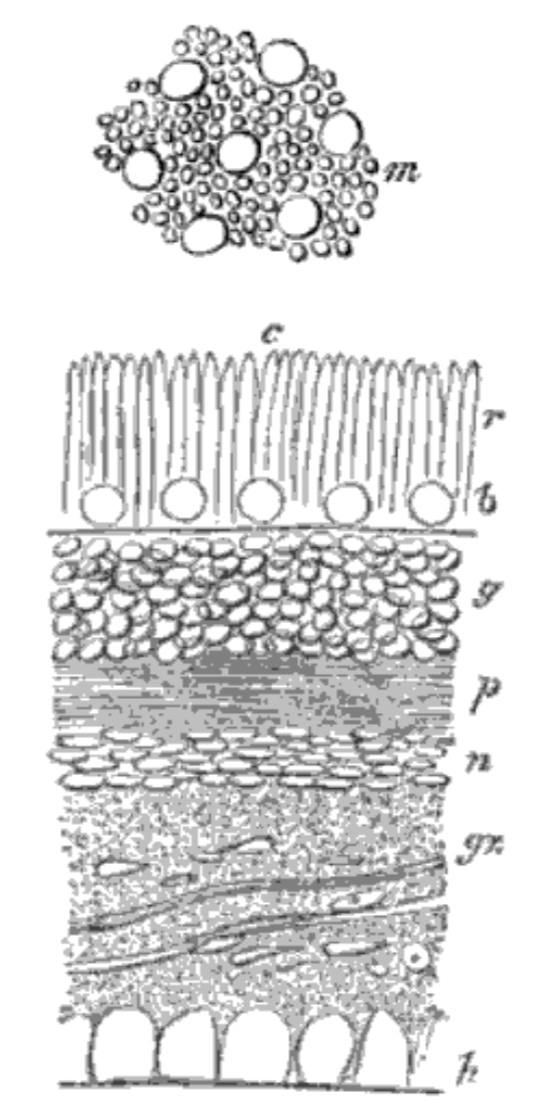
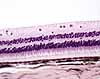
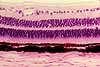 The neural retina consists of several layers, including several types of
cells. (Click on the thumbnail to right to see the layers labelled.)
The neural retina consists of several layers, including several types of
cells. (Click on the thumbnail to right to see the layers labelled.)
Note that "inner" and "outer" in the names of retinal layers refer to the eyeball, not to the surface of the retina.
- The internal limiting membrane (the retina's innermost layer, closest to the center of the eyeball) is a basal lamina separating nervous tissue of the retina from connective tissue of the vitreous humor.
- The layer of nerve fibers contains axons from ganglion cells as they travel across the retina to the optic nerve.
- The ganglion cell layer contains the cell bodies of ganglion cells, whose axons comprise the optic nerve.
- The inner plexiform layer contains dendrites of ganglion cells synapsing with axons of bipolar cells.
- The inner nuclear layer contains the cell bodies of bipolar cells.
- The outer plexiform layer contains dendrites of bipolar cells synapsing with axons of photoreceptor cells.
- The outer nuclear layer contains the cell bodies of photoreceptor cells.
- The external limiting membrane, located between the outer nuclear layer and the receptor layer, is the site of a line formed by junctions between Müller cell processes. The outer segments (rods and cones) of the photoreceptor cells penetrate this outer limiting membrane to contact the pigmented epithelium.
- The receptor layer contains the photoreceptive outer segments of photoreceptor cells (rods and cones).
Historical note: Among the first to describe these layers in microscopic detail was William Bowman (b. 1816), after whom Bowman's membrane of the cornea is named. In 1847, at a time before knowledge of cells and their nuclei had become well-established, Bowman quaintly labelled the inner and outer nuclear layers as the "layer of nummular agglomerated granules" and the "layer of globular agglomerated granules."Historical note: Decades before the function of the photoreceptor layer was established by Heinrich Müller (in 1855), this layer was known as "Jacob's membrane," after Arthur Jacob (b. 1790).
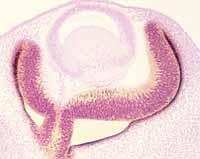
The pigmented epithelium is the outermost layer of the retina, consisting of cuboidal epithelial cells derived from the outer layer of the embryonic optic cup. The dense melanin pigment of this layer absorbs light not captured by photoreceptors. The cells of the pigmented epithelium also contribute to the maintenance of photoreceptors, "recycling" membranes that are shed from rod and cone outer segments.
Clinical note: Although cells of the pigmented epithelium are intimately associated with outer segments (rods and cones) of receptor cells, this surface where the neural retina contacts the pigmented epithelium is inherently extremely fragile. This is the site where retinal detachment can occur.

Three principal neuronal cell types comprise the bulk of the neural retina. For a diagrammatic representation of these three cell types, click on the thumbnail at left.
The spatial density of these three cell types varies across the retina and affects spatial resolution and sensitivity of different portions of the visual field. For a comparison of different retinal regions, click on the thumbnail at right.
Continue reading for further details about these as well as additional retinal cell types.
- Photoreceptor cells come in two types, rods and cones.
- The names "rod" and "cone" are descriptive of the shapes, as seen microscopically, of the outer segments of the photoreceptors.
- Each outer segment is a highly-modified cilium, with many sheet-like folds
of membrane arranged in a tall stack. The outer segments can be properly appreciated
only by electron microscopy. (See the Electron
Microscopic Atlas).
- The outer segments are in intimate association with cells of the pigmented epithelium, which provide support by "recycling" membranes shed from those segments.
- Rods are sensitive to dim light and provide night vision. Rods are more numerous in the peripheral retina.
- Cones need brighter light and provide daytime
color vision. Cones are more prevalent in the vicinity of the
fovea.
- Three different pigments, in three different sub-types of cones, are each optimally sensitive to a different wavelength of light.
- Photoreceptor cells synapse with bipolar cells in the outer plexiform layer.
The retina has received intensive research investigation, so a super-abundance of information is available about the structures and functions of its cells. For additional details, consult your print resources or search the web. (As an example of such research, the journal Nature has published a detailed 3D description of neural connections in the retina of the mouse [Helmstaedter, M. et al. Nature 500, 168-174, 2013]. A video might be found here, if Nature maintains public accessiblity for this link.)
Blind spot
The blind spot is the portion of the retina where the optic nerve penetrates the wall of the eyeball. Here, because there are no photoreceptors, the visual field is blank. We do not notice this blind spot because the region of the visual field which is blank for one eye is imaged by the other eye. Even with one eye closed, the blind spot is inconspicuous because our visual system seems designed to ignore it. Follow the steps below to detect the presence of a blind spot in the visual field of one of your own eyes.
- Cover or close one eye.
- With the open eye, look at a small object (preferably, one silhouetted against a fairly bland background).
- Slowly shift your gaze away from the object, turning your eye horizontally toward your nose.
- When the object is a few degrees to the side of your gaze, it should "disappear."
When an object "disappears" into the blind spot, its image has fallen onto the site where the optic nerve leaves the eye. Here it cannot be "seen" by the retina. But no matter what color the background displays, there is no perception of a "hole" in the visual field. The visual system compensates for the blind spot by "filling in" the corresponding area with a perception that matches the background color.
And of course, when both eyes are open the area of the visual field which falls onto the blind spot of one eye is still seen by the other eye.
The optic nerve is properly considered a tract of the central nervous system, rather than a peripheral nerve, since the retina itself is derived from the embryonic diencephalon (i.e., from neuroectoderm). The axons in the optic nerve come from ganglion cells in the retina. The majority of these axons project through the optic chiasm and optic tract to the lateral geniculate nucleus of the thalamus, but some have other destinations in the brain.
The small area where optic nerve fibers penetrate the retina is a "blind spot," where no image information is collected.